Featured Resources to Address Behavioral Health Needs
Posted by PHN Communications | May 11, 2026 | Star Central
Guide patients to the right level of complex care
To help you more easily connect patients with appropriate behavioral health support, consider these two Optum resources:
Optum Complex Case Management program
This program is designed for members with complex behavioral health conditions who may benefit from intensive service coordination. Care coordinators work closely with patients to develop a comprehensive, individualized plan that connects patients to medical and behavioral care and therapy; community and psychosocial support services; recovery resources; and other needed services, including shelter and basic needs.
Criteria for the program include the presence of a complex behavioral health condition, a history of intensive service utilization over the past 12 months and a willingness to participate. To refer patients, email care.coordination@optum.com.
Behavioral Health Referrals – Provider Types guide
This quick-reference chart outlines behavioral health provider types and the services they offer, helping you match patients with the right clinician based on clinical need.
For example, it clarifies which providers offer psychological testing or interventions or prescribe medications.
Peoples Health Complex Case Management Program
Peoples Health also provides complex case management to Peoples Health plan members with multiple medical or behavioral health conditions and a social situation that affects management of care. The program meets health needs through services provided in accordance with NCQA guidance and established clinical case management practices and standards. Provider referrals can be made by faxing a medical necessity request. Contact your Peoples Health representative for more information.
NEWSLETTERS
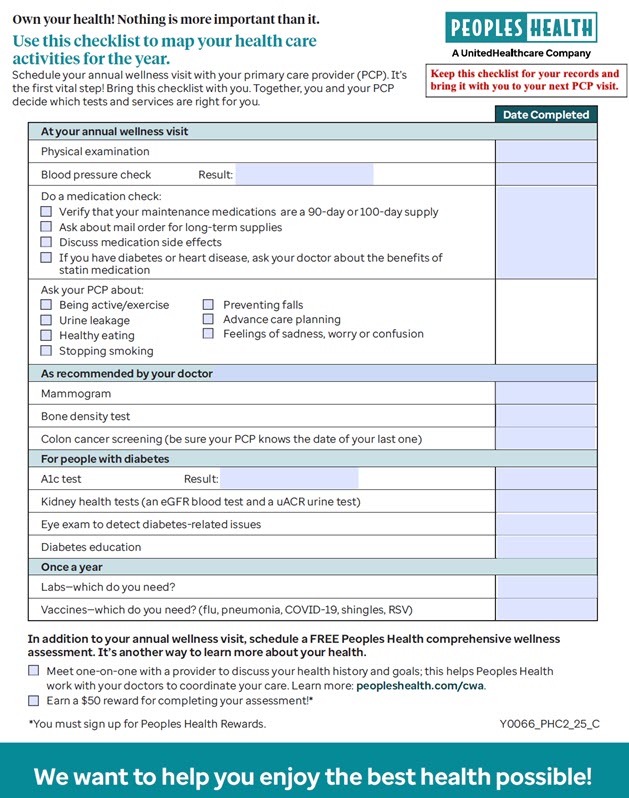
PREVENTIVE CARE
CHECKLIST
EDUCATIONAL VIDEOS


ARTICLES BY CATEGORY
